Keratitis is an eye condition involving the inflammation of the cornea (the clear, outermost surface of the eye).
It may have several infectious or noninfectious causes and can significantly impact eye health and vision.
It is important to seek immediate medical attention if you experience redness, swelling, eye pain, and watery eyes.
This article explores everything linked to Keratitis, including its types, causes, symptoms, and treatment approaches.
What is Keratitis
Keratitis is an inflammation of the cornea, the clear front layer of the eye that covers the iris and pupil.
Infections (bacterial, viral, or fungal), eye trauma, contact lens abuse, dry eyes, or underlying health issues can all contribute to this illness.
Keratitis typically causes symptoms such as eye redness & pain, light sensitivity, impaired vision, and, in rare cases, discharge.
Timely diagnosis and treatment are critical to avoid complications and maintain eye health.
Save up to 90% on your medicine bills
Eyemist Forte 10 ml

Restasis 0.05% Ophthalmic Emulsion 0.4ml

Milflox 0.5% 5 ml

Pred Forte 10 ml
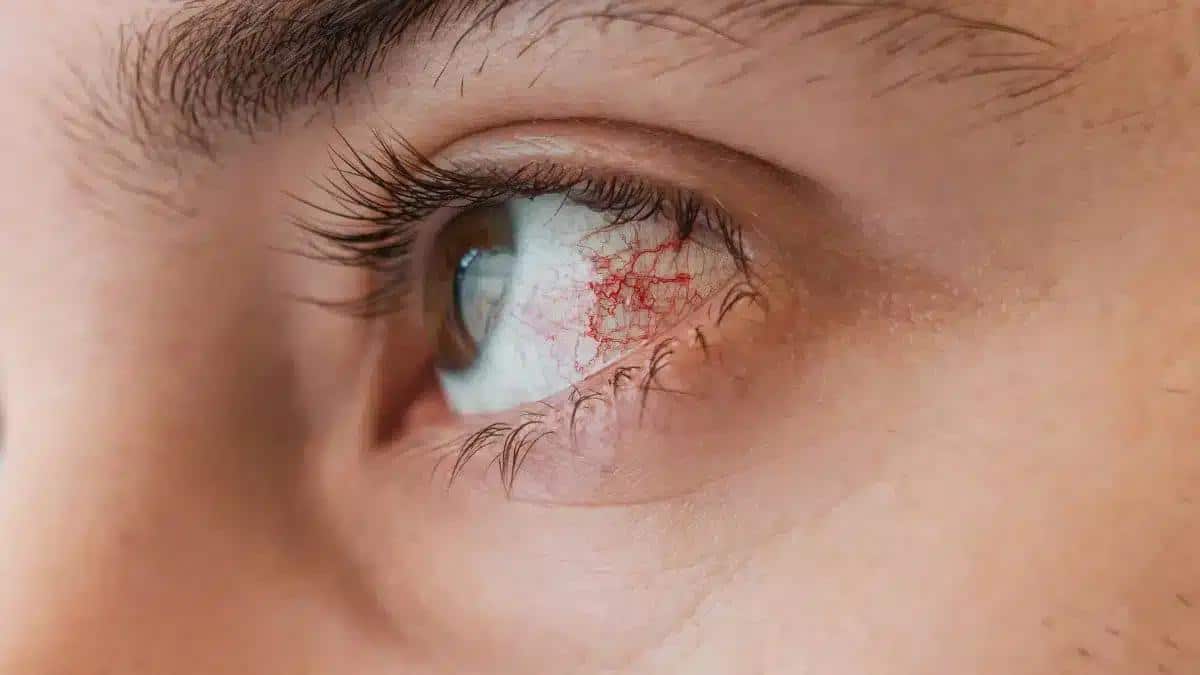
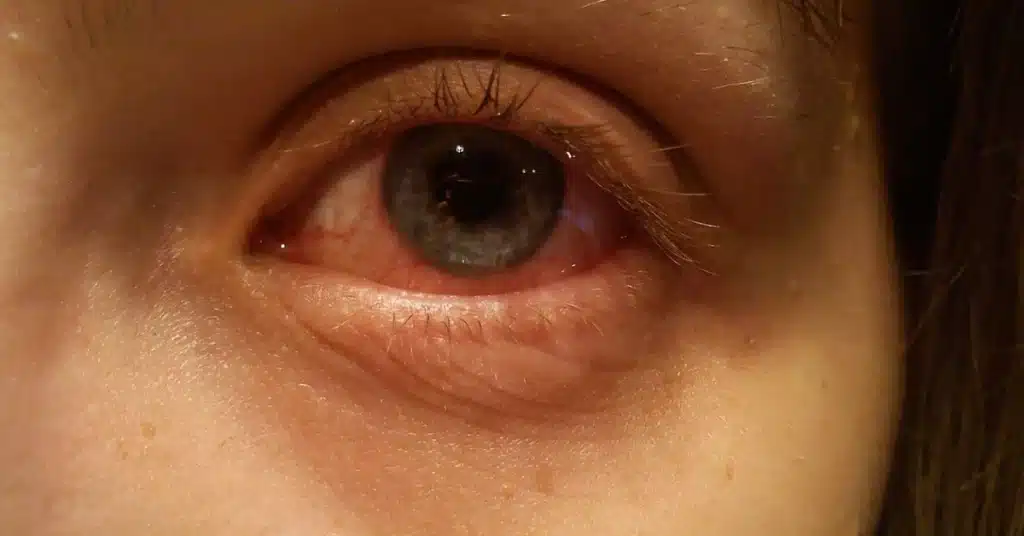
Keratitis symptoms
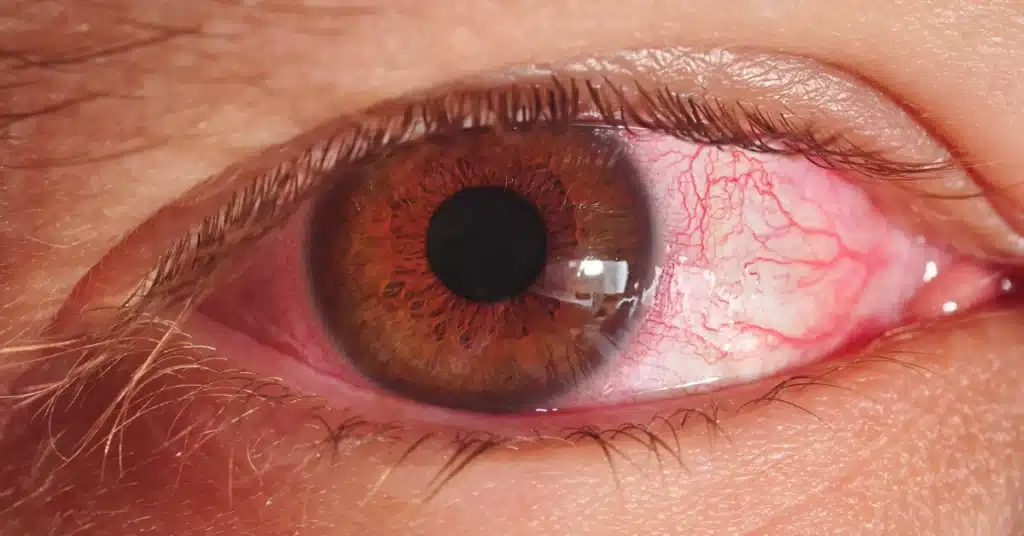 Source: dtimiraos_from_Getty_Images
Source: dtimiraos_from_Getty_ImagesThe symptoms of corneal Keratitis can vary based on the cause and severity of the condition.
However, some common symptoms of the condition are as follows:
- Red eyes and swelling
- Eye pain, discomfort, or irritation
- Blurry or hazy vision due to corneal irregularities caused by inflammation
- Sensitivity to light (Photophobia) in bright environments
- Excessive tear production and discharge
- A sensation of having a foreign object or grit in the eye
Shop at GoodRxMedicine: Eye Care
Types of Keratitis
Keratitis can be classified into various types depending on the underlying causes or the affected areas.
Based on the affected part of the cornea, Keratitis may be Superficial, Deep, or Marginal.
- Superficial Keratitis affects the outer layers of the cornea
- Deep Keratitis involves the inflammation of the deeper layers of the cornea
- Marginal Keratitis develops at the margins or periphery of the cornea.
Let us take a closer look at the types of Keratitis and their subtypes:
Superficial Keratitis
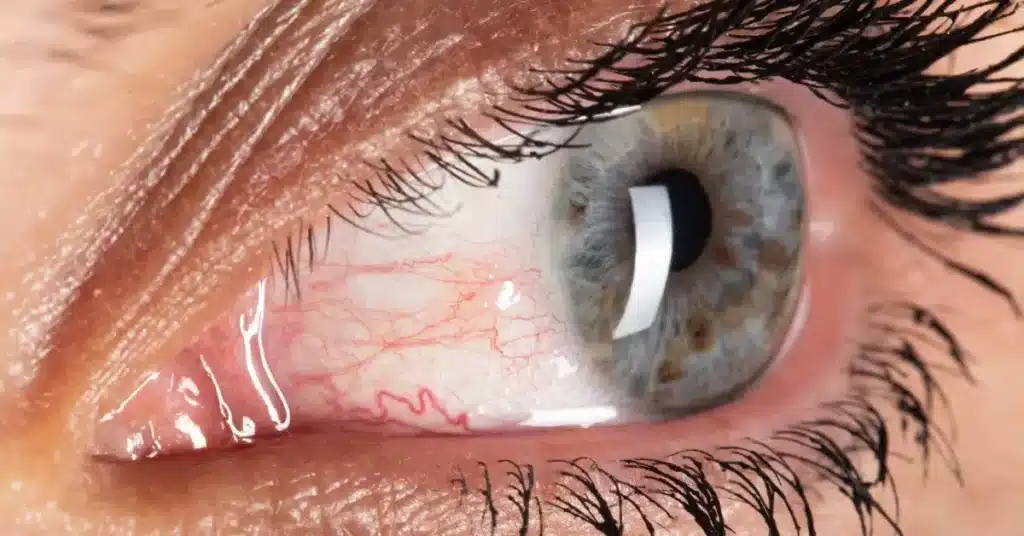
Superficial Keratitis causes inflammation in the cornea’s outer layers, leading to symptoms like redness, blurry vision, and eye pain.
It can occur due to both infectious and noninfectious causes.
Based on the symptoms, this condition can be further classified into Filamentary Keratitis, Punctate Keratitis, and Ulcerative Keratitis.
Filamentary Keratitis: It forms filaments on the corneal surface, leading to discomfort and irritation.
Punctate Keratitis: Involves multiple tiny inflammatory spots on the cornea, often caused by dry eyes or infections.
Ulcerative Keratitis: Infections or other injuries can create corneal ulcers or open sores on the surface.
Deep Keratitis
Deep Keratitis affects the deeper layers of the cornea, leading to potentially severe complications requiring prompt medical attention.
It can occur due to exposure to environmental triggers or nerve damage from underlying health conditions.
It may also develop from complications following LASIK or other medical surgeries (Diffuse Lamellar Keratitis).
It can be further classified into Stromal and Interstitial Keratitis.
Interstitial Keratitis develops beneath the corneal flap and the stroma (the cornea’s middle layer). Stromal Keratitis affects the stroma and the deeper layers of the cornea.
Marginal Keratitis
Marginal Keratitis involves inflammation at the cornea’s periphery, typically near the area between the cornea and the sclera (limbus).
It mainly affects the corneal edges, leading to pain, discomfort, and various symptoms. It is also known as Peripheral Keratitis.
Recommended read: Learn why Marginal Keratitis occurs and how to treat it — Marginal Keratitis: Symptoms, Causes, and Treatment Options
Causes of Keratitis
 Source: Syda_productions
Source: Syda_productionsKeratitis, which leads to inflammation of the cornea, may have both infectious and noninfectious causes.
It can develop from infections caused by microbial pathogens, such as fungi, bacteria, viruses, and parasites.
Non-microbial triggers like injury, eye trauma, and autoimmune diseases can also cause corneal ulcers.
Let us discuss the infectious and noninfectious causes of Keratitis:
Infectious causes
Several bacterial, fungal, viral, and parasitic infections can lead to an infectious type of Keratitis known as Microbial Keratitis.
The common infectious triggers for Keratitis include:
Bacterial infections: Bacteria such as Pseudomonas aeruginosa and Staphylococcus aureus often lead to Bacterial Keratitis, also known as a corneal ulcer.
Viral infections: Viral Keratitis can develop from viruses such as Herpes Simplex Virus or HSV (which causes Herpes Keratitis) or Varicella-Zoster Virus (VZV).
Fungal infections: Fungal Keratitis may occur due to infections of Fusarium, Aspergillus, or Candida.
Parasitic infections: A one-celled parasite called amoeba can lead to a rare but severe infection known as Acanthamoeba Keratitis.
Infectious Keratitis can be contagious, depending on the specific pathogen. It can spread from direct or indirect contact with affected individuals.
Medical conditions that impair the immune system can make individuals susceptible to infections.
Swimming while wearing contact lenses can expose you to bacteria and parasites in water bodies, leading to infections.
Eye injuries caused by scratches from a tree branch or other plant parts can lead to Fungal Keratitis. People who work on farms are more prone to developing this infection.
Recommended read: Learn everything you need to know about infectious Keratitis —- Microbial Keratitis Unveiled: Causes, Symptoms, and Treatment Options
Noninfectious causes
Corneal ulcers and swelling in the eye can also occur due to surgery, injuries, or diseases, even without an infection.
The primary causes of noninfectious Keratitis include:
Improper contact lens wear: Poor hygiene, contaminated lenses, or wearing contact lenses for prolonged periods (or while sleeping) can lead to corneal dryness, scratching, and dryness.
Environmental factors: Long-term exposure to environmental triggers, such as UV rays, sun, wind, light, dust, or chemicals, can lead to Exposure Keratitis.
It occurs when the eyelid doesn’t close properly, leading to corneal drying and damage.
Nerve damage: Damage to the nerve due to underlying health conditions or complications after surgery can lead to Neurotrophic Keratitis. Diabetes, Trigeminal nerve injury, and postoperative issues after neurosurgical procedures are common causes.
In addition, noninfectious Keratitis can occur due to:
- Eye injury
- Allergies
- Foreign object in the eye
- Autoimmune disorders
Below is a table classifying various Keratitis types into infectious and noninfectious causes.
| Classification | Keratitis type | |
| Infectious | Superficial(Punctate or Ulcerative) | Bacterial Keratitis |
| Fungal Keratitis | ||
| Viral Keratitis | ||
| Acanthamoeba Keratitis | ||
| Deep | Herpes Keratitis (Interstitial or Stromal) | |
| Syphilis (Interstitial) | ||
| Noninfectious | Superficial (Filamentary) | Exposure Keratitis |
| Neurotrophic Keratitis | ||
| Deep | Exposure Keratitis (Interstitial) | |
| Neurotrophic Keratitis (Interstitial) | ||
| Diffuse Lamellar Keratitis (Stromal) | ||
Recommended read: Wondering why Keratitis occurs? Check out — Keratitis Causes: Discovering What Leads to Corneal Inflammation
Treatment of Keratitis
Keratitis treatment varies depending on the underlying cause, severity, affected area, and type of Keratitis.
Antimicrobial medicines may be prescribed for treating Keratitis. Alternatively, noninfectious Keratitis requires various treatment approaches that address the underlying cause.
Consulting an eye specialist is essential for an accurate diagnosis and appropriate treatment.
Immediate treatment is necessary to prevent complications.
People who wear contact lenses are usually recommended to stop using them until the infection clears to avoid worsening the condition.
Let us look at potential treatment options for Keratitis:
Medications
Doctors may prescribe specific oral or topical medicines to combat viral, bacterial, and fungal infections. Specific antivirals like Acyclovir and Ganciclovir can help treat Viral Keratitis.
Antibiotics like Tobramycin, Doxycycline, Ciprofloxacin, and Moxifloxacin can help fight bacterial eye infections.
Corticosteroids may reduce inflammation in noninfectious cases, although they are avoided in infectious cases.
In addition, lubricating Keratitis eye drops can help keep the eye moist and promote healing.
Preservative-free eye drops are used to minimize irritation, particularly in cases of Neurotrophic Keratitis or Peripheral Ulcerative Keratitis.
Surgery or Procedures
Some severe cases of Keratitis may necessitate surgical procedures to treat corneal damage.
Common surgical procedures that help treat Keratitis include:
Corneal debridement: This procedure involves the removal of diseased tissue or debris from the cornea to aid in healing.
Corneal transplant (Keratoplasty): A corneal transplant may be necessary in severe cases or when other treatments fail.
Summing up
Keratitis is an inflammatory condition that affects the cornea, the front dome-shaped surface of the eye.
It causes various symptoms depending on the underlying cause and affected area. Red eyes, swelling, blurry vision, eye pain and sensitivity to light are common indicators of the condition.
Based on the affected corneal layer, Keratitis may be superficial (outer layer), deep (deeper layers), or marginal (periphery).
It can develop from infectious (bacterial, viral, fungal, and parasitic) or noninfectious causes (environment exposure, nerve damage, surgical complications).
Treating Keratitis involves using various oral medicines to fight infections and eye drops or ointments to reduce inflammation.
Surgical procedures like corneal debridement and keratoplasty may be necessary in severe cases when all treatments fail.
It is important to consult an eye specialist if you experience symptoms. Neglecting your symptoms can lead to potential vision complications.

Frequently Asked Questions
How long does Keratitis last?
The duration depends on the cause and severity. With timely treatment, mild cases of Keratitis may resolve within a few days to a couple of weeks. However, severe or recurrent cases may persist longer.
What does Keratitis look like?
The visible symptoms of Keratitis include eye redness, swelling, and excessive tearing. It also causes eye pain, blurry vision, light sensitivity, and a sensation of a foreign object in the eye.
The symptoms depend on the underlying cause and may vary from person to person.
Is Keratitis serious?
The severity of Keratitis depends on the underlying cause. The condition should be taken seriously, as untreated cases can lead to corneal damage or permanent vision loss. Seeking immediate medical attention is critical.
Can you recover from Keratitis?
Yes, recovery from Keratitis is possible with prompt and effective treatment. Mild cases usually resolve on their own, but severe or recurring cases may necessitate extended treatment and regular monitoring by an eye care specialist for a full recovery.
When referencing outside resources, GoodrxMedicine always provides full citations. To learn more about the measures we use to maintain the quality of our content, please review our Content Information Policy.